| Claire Laurent, Author and Journalist | The UKAHN Bulletin |
| Volume 8 (1) 2020 | |
I entered nurse training at the tail end of an era in which entry requirements could be fairly bizarre: from the quality of your needlework skills, the provision of a photograph of yourself, to a reference (or three) from a reverend. Where you went to school and what your father did for a living were also considered relevant. I suspect that having generations of nurses, doctors and midwives in my family helped me take up a place, despite the absence of Maths O level – a crucial requisite today.
Nursing is steeped in tradition; custom and practice handed down from generation to generation, learning absorbed at the bedside. My training in the early 1980s at St Bartholomew’s Hospital was not so different to my mother’s at the same hospital in the 1950s. For sure, we had marginally less cleaning to do, the discipline was a little more relaxed, and senior nursing officers took the place of matron but the ward processes and procedures remained similar.
For the best part of the twentieth century, nurses were paid members of the ward. We had an apprenticeship style of training: our ward placements of three months or more were interspersed with two weeks in the classroom – ‘in block’.

These days, new recruits for nurse registration require three A levels to start their degree courses. Their training is split 50/50 between lecture theatre and supervised supernumerary ward placement and with the withdrawal of the student bursary, they pay £9,000 plus a year for their courses.
The eminent American nurse, Virginia Henderson, whose theories strongly influenced nursing on both sides of the Atlantic during the twentieth century, is quoted in 1967 as saying:
Most aspects of basic nursing, including the nurse’s approach to the patient are steeped in tradition and passed on from one generation of nurse to another. Too often they are routine without rhyme or reason. They are learned by imitation and taught with little if any reference to the underlying sciences.1
Nearly twenty years later, this lack of rhyme or reason was still the case. Hard as our tutors urged us to challenge poor practice on the ward, we rarely did. The risk of querying anyone more senior than yourself and still surviving your placement was too great.
Salt baths, often known as sitz baths are a good example: in block we might learn the exact ratio of salt to water to ensure a ‘therapeutic’ bath (itself something of a myth) only to find that on the ward you just tossed a cup of salt into the bath, no measurement required.
There are a number of books exploring rituals and myths in nursing and generally their authors fall into one of two camps: those who slate rituals as undermining practice by lack of evidence and applied without thought, while others find good in some rituals because, they provide, comfort, reassurance and routine.
Bed baths fall into this latter category – offering patients comfort and the nurse a chance to observe and listen to her patient. Bed baths followed a strict process: curtains pulled around the bed and an explanation given to the patient. Top bedclothes were folded back in thirds to the foot of the bed, keeping the patient covered. We carried a bowl of warm water to the bedside (on a tray). The wash started with the patient’s face and worked methodically down the front, change of water and then their back, ‘log rolling’ the patient if they were unable to move themselves. Towels and a sheet always strategically placed to ensure patients were kept warm and not exposed.
Mike Walsh and Pauline Ford in their 1989 book Nursing Rituals, research and rational actions decried rituals in nursing practice and noted that some verged on witchcraft and had their origins in the mythology of nursing.2 For many people, the application of leeches and maggots might be said to fall into this category. Medicinal leeches are used to relieve an area congested with blood by sucking it up. They have three jaws of tiny rows of teeth, which pierce a person’s skin and insert Hirudin, a substance that prevents blood clotting allowing them to easily remove the blood from the congested area. Leeches can be applied to patients undergoing plastic surgery or who are at risk of losing a limb. They can also treat blood clots, varicose veins and dangerously high blood pressure.
Ann Lamb, a nurse at the Royal Infirmary Edinburgh in 1932, noted that ‘the average leech will draw off 1 oz of blood’ demonstrating their effectiveness at relieving congestion. She observed that and that to apply leeches ‘the skin must be clean but free from soap. A drop of milk may be dropped over the part to be treated and nurses must watch that the leech does not wander, having taken the precaution to ‘plug all adjoining cavities!’ Modern Professional Nursing (circa 1942) warns that a leech has to be: ‘humoured before he will consent to perform…’. Modern medical leeches are especially bred, sanitised and cost a £1,000 per batch.
Maggots also have a medical use, but being often associated with dirt, are harder to contemplate for good. However, using them to clean wounds dates back centuries with each generation discovering their powers, particularly in wartime when soldiers with wounds infested with maggots did better than those that hadn’t. One student nurse I knew, was castigated for cleaning all the maggots out of the wound of a homeless man admitted into the hospital when she helped him to wash. The maggots were helping to heal the wound, even if they hadn’t been put there deliberately. Maggots are still sometimes used for wounds that won’t heal. Research has shown that their secretions contain an enzyme which can kill bacteria thus they disinfect as they clean, producing a dual action; they also stimulate the development of healthy tissues.
Prior to degree course nursing, procedure books were on every ward offering guidance on anything from giving an enema to dressing a wound. They were often based on the idiosyncrasies of the ward sister or the consultant rather than scientific evidence, because as Walsh and Ford pointed out: ‘Ritual and tradition are not the sole prerogative of nurses.’
Operating theatres have plenty of their own rituals. In the past, surgeons felt they had only ‘arrived’ as consultants when they had their own book, full of rituals that nurses, theatre technicians and junior doctors had to follow. As the lowest of the low, student nurses in theatres generally kept out of the way, stocking cupboards, shelves and linen cupboards, hoping not to attract attention as they tried to learn custom and practice by osmosis. Theatres were only friendly if you were part of the ‘clique’ and student nurses rarely were. In an interview, Linda, who trained in the 1960s told me ‘It was impossible for me to walk across the floor of theatre without tripping over a piece of equipment, contaminating the sterile field, or knocking over a tray of instruments.’
There were some rituals prior to surgery which we hung onto and perhaps overplayed. The traditional shave was one of these. Its purpose was to reduce the risk of infection when a surgical incision was made. However, apart from the embarrassment to all parties because the shave is usually in an intimate area of the body, the irony is that the shave itself could cause cuts or abrasions which could be a source of infection. Pre-op shaving is rarely done these days.
Preventing pressure sores has been a caring ritual since they were first recorded as far back as ancient Egypt. Arguments as to their cause and, more pertinently, who is to ‘blame’ for them have been around for ever. As Clara S Weeks reports in Text Book of Nursing, 1896; ‘Bedsores are frequently occasioned by bad nursing, and cases are rare in which good nursing cannot avert their formation’.3 This view was fuelled during the nineteenth and twentieth century by the mistaken belief (developed by a 19th century French neurologist) that pressure sores were an unavoidable result of damage to the brain or spinal cord.4 This theory persisted until the 1940s, which meant that the medical profession was sceptical about the chances of preventing and treating the ulcers and so left the care of them to nurses.
The role of compression of the skin only came to be understood later and, with it the realisation that those who were immobile were particularly at risk from such compression. Prevention remains key, because once pressure sores develop, they are, as the weird remedies used to treat them are testament to, very difficult to resolve. The most common prevention technique, which became known as ‘the back round’ involved helping patients regularly to move position. Ida, who began her training at the Royal Infirmary Edinburgh (RIE) in 1918, recalls the back round in her account held in the RCN oral history collection:
…nurse said to me ‘Go and get the back tray’. So, I rushed off to the kitchen and brought out a big black tray (and) put it under the bed … I caused confusion I can tell you. It was the back tray for doing the backs, you see (that she wanted)
In my Aunt Molly’s day in the 1940s, the back round remained a strict regime, the three essential rules of which were: maintain absolute cleanliness, avoid prolonged pressure and stimulate the circulation of the part.
Patient cleanliness involved a wash twice a day, or every time the patient was incontinent. After washing, the nurse soaped her own hands well (there were no gloves in this period) and rubbed the suds into the patient’s back until it was absorbed, leaving the skin dry. Next, she tipped methylated spirit into her hand and rubbed it into the skin until it was pink and dry. Lastly, she rubbed in starch powder (later talcum powder), paying special attention to the fold of the buttocks. Sometimes zinc and castor oil ointment or boracic ointment was used instead of the methylated spirit. Molly doesn’t say what this variety of potions did to her hands, never mind the patients’ skin.
Once a pressure sore developed, all manner of remedies might be applied, from insulin and oxygen to Marmite! A combination of egg white and oxygen was popular from the late 1970s to the early 1990s. It involved smearing egg white onto an open bed sore and drying it with high flow oxygen via a strategically placed oxygen mask.
Prevention and treatment of pressure sores continued to be ritualistic and haphazard until the late1980s when City and Hackney Health Authority’s Chief Nursing Officer, Pam Hibbs carried out a pioneering ten-year study of pressure sores which did much to transform our understanding and the nursing care of pressure sores, ensuring earlier intervention in A&E and in theatre to prevent long hours on trollies or theatre tables which contributed to skin damage.
Most rituals, though, were harmless and helped you work quickly and safely – beds stripped and made in a certain way, wheels all turned in to avoid tripping over them.
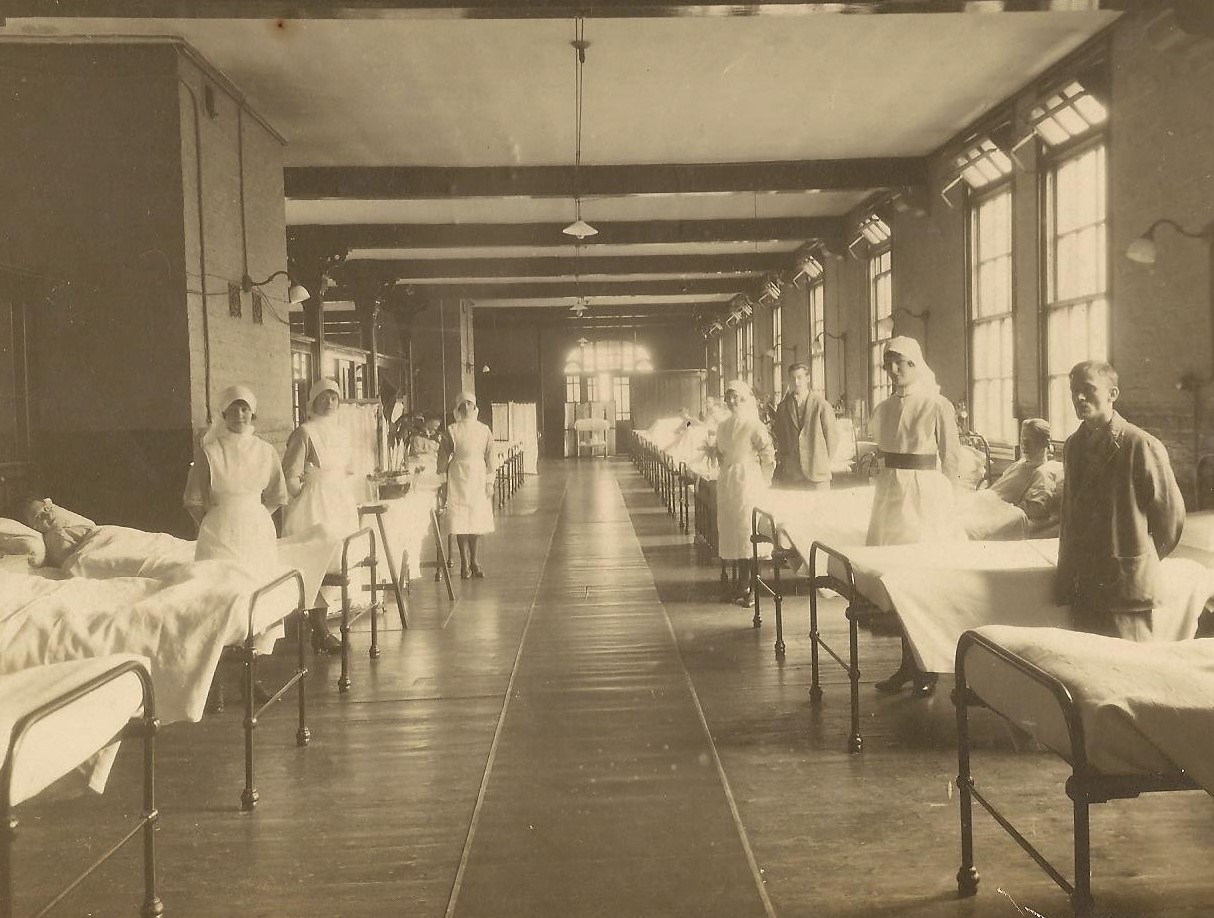
The requirement for pillowcases to open away from the door stemmed from Florence Nightingale’s days in the Crimea, protecting patients from the dirt and dust of war and yet was continued practice throughout the twentieth century. Any nurse who trained in the 20th century will inevitably still make a bed in this way – at home or at work.
Uniforms, badges and hats remained important to the profession long after Florence Nightingale’s original designs. Skirt length and fabric may have changed over time but the basic style of an impractical dress and a white starched apron, with a cape with red straps crossing over the front, topped by a hat remained the mainstay of a nurse’s appearance for more than 100 years.
Nursing schools accorded hats all kinds of status depending on height and whether they had ribbons and frills. Promotion came with a new hat which was presented to nurse by matron: Jan, who trained the old Queen Elizabeth hospital in Birmingham in the 1960s, remembers proudly striding down the corridor after this ceremony, admiring her completely impractical hat in the glass of the ward door. Inevitably, nurses adapted the uniform for their own uses. It was almost ‘de rigeur’ for nurses to smoke for much of the twentieth century: one nurse at Manchester Royal Infirmary reported that there was only time for three puffs of a cigarette at break, so you cut off the end neatly with scissors and popped it in the front fold of your cap for safe keeping. “We must have stank of cigarettes,” she said, “but then so did the patients”.
Ash trays featured on patient lockers until the mid-1970s and in one East End hospital, junior nurses on elderly care wards rolled cigarettes at night for their charges to smoke during the day.
Alcohol formed one of the more unexpected rituals on a ward. When I trained in the 1980s, drug trolleys included beer, sherry and brandy, with bottles and cans of Mackeson’s. Jean, who trained at St Bartholomew’s Hospital recalls:
In 1958 we took the drinks trolley round at 11:30 – to tempt the patients’ appetites and up their iron levels. I got shouted at by an elderly patient on my first ward for not tipping the glass and pouring the Guinness slowly. They did not teach us that at PTS (preliminary training school)!
Brandy was given on the vascular wards to encourage blood flow, while beer was commonly used to persuade men on surgical wards to drink more fluids. Pregnant women were encouraged to drink stout for its iron content, gin encouraged people to pee after surgery, and sherry was used as an appetite stimulant for older patients. Alcohol has made something of a modern day return to wards for older patients whose patients may be dependent on a nightcap at home and might otherwise develop withdrawal symptoms.
Alongside alcohol and regular drugs, there were some potions that were credited with an almost mystical power. The Brompton Cocktail was one of these. It is thought to have derived from a mixture created by a surgeon, Herbert Snow, in the 1890s and given for pain and as a ‘pick you up’ to patients who were terminally ill. Its ingredients varied slightly over the years but essentially it consisted of morphine, alcohol and cocaine mixed with water and syrup and sometimes an anti-sickness drug.5 I remember administering it in the 1980s with a sense of relief, knowing that the patient’s pain would be controlled and that they would experience something of a ‘feel good’ factor.
It has been said that the mixing of substances and liquids is a ‘medicine of faith rather than fact’ and perhaps that describes much of the ritual and myth in nursing – an instinct for and faith in what works. The (very) gradual demise of the Brompton Cocktail can be seen as part of the move to evidence-based medicine and a much greater sophistication in end of life care.
Many of these practices evolved over time. Learning by imitation and anecdote is powerful. Much of the time when I started out we did things because Sister said so and if it appeared to work, so much the better. Student nurses today are taught to question and to understand why they do things. That can’t be bad but no doubt they will be just as nostalgic for the strange things they did in good faith along the way.
This article is based on a new book, Rituals & Myths in Nursing by Claire Laurent, published in 2019 by Pen & Sword.
References
- Stephanie Hamilton Smith, ‘Nil by Mouth?: A descriptive study of nursing care in relation to pre-operative fasting’, Royal College of Nursing (1972). Accessible as pdf from RCN website (last accessed 29 December 2019).
- Mike Walsh and Pauline Ford, Nursing Rituals: Research and Rational Actions (Oxford: Butterworth Heinemann, 1989).
- Clara S Weeks, A Text-Book of Nursing (New York: D. Appleton & Co, 1896), p.49.
- Jeffrey M Levine, ‘Historical perspective on pressure ulcers: the decubitus ominosus of Jean-Martin Charcot’, Journal of the American Geriatric Society 53/7 (2005), pp.1248-51. Accessed online https://www.ncbi.nlm.nih.gov/pubmed/16108947
- Professor David Clark, ‘The Brompton Cocktail: 19th century origins to 20th century demise’ University of Glasgow (2014) Accessed online http://endoflifestudies.academicblogs.co.uk/the-brompton-cocktail-19th-century-origins-to-20th-century-demise/
